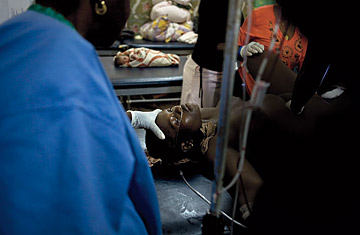
After giving birth in the Princess Christian Maternity Ward in Freetown, Sierra Leone, Conteh underwent emergency treatment as her infant lay nearby.
(2 of 2)
More will die if health-care systems are not reformed. In the first half of this year, 889 babies were delivered in Freetown's crumbling Princess Christian Maternity Hospital. During that period, 70 women died giving birth, and about eight more women have died since--an astonishing death rate of about 9%. Yet far from being overstretched, the hospital most days feels desultory, with nurses lingering in near empty wards because people cannot afford to pay for care. Emergency maternity care is supposed to be free in Sierra Leone, but in reality, patients are asked to pay for every item, including cotton swabs, gauze and syringes--this in a country where the average income is about $200 a year. If transfusions are needed, relatives have to donate blood to replace what is used.
One morning I watched a fierce argument between nurses and the relatives of a woman whose unborn baby was already dead inside her. As she sat on a bed awaiting an emergency C-section, her relatives pleaded that they could not afford 400,000 leones (about $135) for the operation. Finally the woman's aunt handed some 250,000 leones (about $85) to a nurse, who counted the banknotes before jamming them into her pocket, explaining to me that the money was "for drugs and to pay the doctor." Since nurses and doctors earn about $150 a month, "the staff is struggling to survive," says Peter Sikana, technical adviser for the U.N. Population Fund in Sierra Leone.
The scribbled notes from nurses in patient records, many of them in school exercise books paid for by relatives, describe their battles to keep women alive. In one such note, a nurse describes a woman, 18, who arrived at the hospital in late July suffering convulsions days after a traditional birth attendant delivered her baby at home. Four days later, the nurse wrote, "All due nursing care rendered but in vain. May her soul rest in peace." Six weeks later, I find the woman's father sitting outside the tiny family home atop an escarpment that overlooks Freetown. Holding the newborn baby, he says his daughter gave birth at home because "the terrain is too rough to reach the hospital." By the time he carried her, half conscious, down the slope to the hospital, she was too sick to be saved. Even for women who give birth in a hospital, survival is no sure thing. Another woman, 20, was admitted in late July in early labor and began having seizures hours after giving birth. Through the night the nurses scrawled frantic notes, including this one at 1:30 a.m.: "Dr. was tried ... via mobile [phone] to no avail." The woman died two hours later. I find her husband grinding peanuts in a Freetown market. "She delivered a healthy baby," he says, showing me a photograph of his wife, a tall woman with a confident, beaming smile.
Hope, for Some
Though many die in hospitals, researchers say the riskiest births are those without any nurse, midwife or doctor in attendance--about 35% of all the world's births. In addition to age-old problems like unclean instruments and poor-quality water--in Sierra Leone, I visited a traditional birth attendant who said she had delivered hundreds of babies in a windowless room in a slum of cramped shanties, with no indoor plumbing--there are new hazards. Afghanistan, for example, has seen growing sales of over-the-counter oxytocin, an injectable hormone that is used to stanch postpartum bleeding and speed labor but that can kill if administered incorrectly. Shamisa, a midwife, says that recently a heavily pregnant woman was brought to her rural Badakhshan clinic in a coma after being given a range of drugs by a pharmacist; both she and the baby died.
After millions of deaths and years of muddled government policies, a groundswell of distress at maternal mortality rates is at last stirring action. At the July G-8 summit of industrialized nations in Hokkaido, Japan, leaders for the first time discussed maternal deaths as a crucial obstacle to development. And there has been progress. Some poor countries have shown rapid results from investments in maternal health: in Honduras, for example, maternal mortality rates dropped about 50% from 1990 to '97 after officials opened scores of rural clinics and trained thousands of midwives. Nepal and Sri Lanka have trained midwives in emergency obstetrics. In the Indian states of Assam, Madhya Pradesh and Orissa, pregnant women now get 1,400 rupees ($32) to spend on whatever maternity services they choose--even a taxi ride to a clinic to give birth. Afghanistan has built 1,465 clinics and trained about 19,000 community health workers since the Taliban was ousted in 2001. The incidence of this worldwide tragedy can be reduced.
Even in Sierra Leone there are glimmers of hope. Aid organizations recently began training traditional birth attendants; several towns now demand that they deliver babies in clinics, where nurses can monitor their work. An hour east of Freetown, I visited a village where local elders had just passed a law requiring all women to give birth at a clinic or face fines of about $8--more than the clinic fee. And the World Bank, UNICEF and the British government's Department for International Development have agreed to jointly invest $262 million over the next three years to overhaul Sierra Leone's shambolic health system. "We will lose two or three more generations," says Geert Cappelaere, UNICEF's representative in Freetown. "But the core message is one of hope."
For some, that hope has come too late. A week after Conteh's death, her relatives gathered to name her baby girl after the dead mother. Weeping, Conteh's parents and her boyfriend hugged and kissed the infant, a bittersweet reminder of their loss. They are not alone. In the time it has taken to read this story, about 20 more women have died in childbirth.
