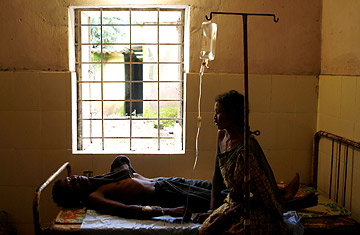
An Indian patient is treated for suspected cholera in a hospital in Kakiriguma village of Koraput district, some 500 kilometres southwest of Orissa state's capital, Bhubaneswar.
Correction Appended: Sept. 2, 2008
India's vast skilled workforce gets western companies' jobs done cheaper and faster. Much has been written about the outsourced back-office services — in IT, finance, telecom — that have helped propel the country's growth to more than 8% a year (and elicited backlash in the countries that buy them). Now a lesser-known western industry has begun tapping India's outsourcing pool, prompting concerns not about jobs, but about the health and safety of the Indian population: Big Pharma.
The price of bringing a new drug to market is, on average, $1 billion. The bulk of that cost is devoted to human clinical trials — the most crucial and time-consuming phase of drug development. Faced with tight regulations at home and shrinking profits due to expiring drug patents, western drug makers are looking to expedite the process by outsourcing safety and efficacy studies to developing countries, a large proportion of them to India. An amendment proposed last year by the technical advisory committee of India's Health Ministry would further allow drug companies to test their products widely on patients in India before they're proved safe at home, which is causing alarm among sections of civil society. It would be a dangerous situation even in developed countries, but potentially devastating in a country that lacks the medical infrastructure to care for people harmed by untested drugs.
The outsourcing of clinical trials gained pace roughly a decade back; since than, many questions have been raised about it. There are currently some 400 clinical trials underway in India, where the business is expected to be worth $1 billion to $1.5 billion by 2010. For western drug companies, it's a boon: India's vast pool of qualified, English-speaking doctors and lower labor costs make clinical trials up to 50% to 60% cheaper here. Beyond the savings in cash, India offers a crucial savings on time. A drug patent lasts 20 years; during the first seven or eight years of that period, typically, a new drug is tied up in several rounds of human clinical trials. That leaves little time for the drug maker to market and profit from the product. To speed up trials, pharmaceutical companies need to recruit large numbers of subjects quickly, something that is often not possible in western countries, where most patients have health insurance or government benefits and are reluctant to sign up. In India, by contrast, much of the population has no health insurance, and public health services are dismal; the promise of getting regular medical attention by enrolling in a trial is often too valuable to pass up. "Many patients in India enter into clinical trials because they have no better option to receiving care," says Sonia Shah, author of The Body Hunters: How the Drug Industry Tests Its Products on the World's Poorest Patients. "That is by definition a coercive situation."
Further, many Indian patients who sign up for trials are illiterate, and it is difficult to ascertain whether they have properly understood the consent documents. "One of the major problems of clinical trials in India is that they are not publicized as clinical trials," says Dr. Chandra M. Gulhati, editor of the civil society journal Monthly Index of Medical Specialties. He says despite regulations to ensure otherwise, most patients are not informed by physicians that they are taking part in a trial. "Physicians are attracted by inducements of foreign travel, funds and fame. Of the four stakeholders — the sponsor or drug company, hospital, investigator and patient — three are on one side," says Gulhati. "They are only interested in getting the trial done."
As is often the case in India, government regulation has followed, rather than anticipated, the flow of business. Already, toxic drugs have posed problems: in 2002, a trial in India, along with 31 other countries, of Novo Nordisk's diabetes drug ragaglitazar had to be suspended after a trial in mice revealed that the compound caused urinary bladder tumors. In 2003, news circulated that researchers from India-based Sun Pharmaceuticals had given the anticancer drug letrozole to 430 young women to see if it would induce ovulation, despite the fact that the drug is known to be toxic to embryos.
Advocates of clinical-trial outsourcing say the solution is not to prohibit trials — and drive away business — but simply to improve monitoring. Indeed, in 2005 the rules governing clinical trials in India (which fall under Schedule Y of the Drugs and Cosmetics Act) were revised and strengthened, according to guidelines from the International Conference on Harmonization as well as the World Health Organization's Global Clinical Practices, bringing Indian standards up to par with the rest of the world. But even today, industry watchers say, enforcement of these rules in India remains largely inadequate. The office of the Drugs Controller General of India (DCGI), which is tasked with evaluating trial protocols — the detailed study plans that explain a trial's objective, design and methodology — is understaffed and undereducated, Gulhati says. Only a small proportion of DCGI investigators have been trained in good clinical practices; a 2005 count by Gulhati put the number at 200, and he says not much has changed since then.
But those who favor the proposed Pharma-friendly legislation insist that the benefits of allowing the industry to flourish outweigh its costs. "Why should we keep India behind everyone else? Why close our doors for business when we have the capabilities?" asks Brijesh Regal, CEO of Apothecaries Ltd., a New Delhi–based clinical-trial outsourcing firm, referring to India's supply of 600,000 qualified practicing physicians, 14,000 general hospitals and over 170 medical colleges. "Since trials for foreign sponsors must follow international rules, they actually help raise Indian standards. The experience with other outsourcing industries has also been that more business has brought better regulation and monitoring."
Regal adds that competition for clinical-trial dollars ensures that Indian standards remain high, "or western sponsors will simply abandon you." Other advocates note that outsourced trials bring new technology, treatments, diagnostics and drugs to India, thereby advancing the local standards of medical and clinical research. "Companies spend resources to train people and bring in expensive equipment," says Dr. Anil Kukreja, medical director at Roche India, which has more than a dozen trials underway in India, and whose blockbuster breast-cancer drug Herceptin was tested here. "Over time, as the overload from big institutes flows to smaller ones in second-tier cities, the benefits will spread farther."
To critics, that picture is only half-painted. While India does have 600,000 doctors, only a tiny proportion graduated from world-class institutes; many have degrees of dubious merit. And sponsors' or drug companies' oversight is no guarantee that trials will be conducted ethically or safely. It is also unclear whether the presence of outsourced trials will benefit India's medical standards more generally. "Conducting clinical trials is not like landing a man on the moon," says Gulhati. "Those who say it will enable India to develop cutting-edge technology are talking nonsense."
There are even those within the pharmaceutical industry who opt for caution. "We are excited but careful," says Dr. Sanjeev Ahuja, a senior vice president in the medical and regulatory department of Eli Lilly India, which has safely conducted 15 trials in India over the last five years. "Regulators need to work overnight. They need more investigators." Roche India's Kukreja agrees, saying that companies and regulators both need to be "a little bit careful so as not to bring disrepute to the industry and country."
In the face of raging controversy, DCGI's Dr. Surinder Singh clarified in July that only a few select centers in India will carry out human trials of foreign drugs that have not been tested for safety at home. "We are not in a hurry. Patient safety is our prime concern," Singh told reporters in New Delhi.
As the author Shah points out, "In the U.S., there are still problems [with clinical trials,] and there have been 40 years of building this infrastructure. In India, it is nascent, and yet there is a boom in trials nevertheless." In this case, it seems the best pace of reform is not the fastest.
The original version of this story stated that Dr. Sanjeev Ahuja's position with Eli Lilly was associate medical director. Rather, Ahuja is a senior vice president in the medical and regulatory department of Eli Lilly India.
