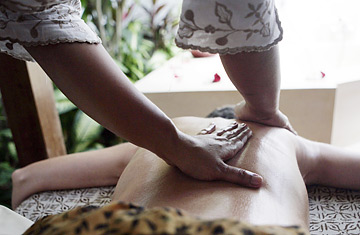
A man receiving a massage treatment.
If you know someone who's getting ready to go into surgery, consider holding off on the get-well-soon balloons, and start looking for a good massage therapist instead. A new study published in the December issue of the American Medical Association's Archives of Surgery found that massage, in conjunction with regular pain medication, significantly improved patient pain and anxiety after major surgery.
The study, which was funded by the Department of Veterans Affairs (VA) and lasted from 2003 to 2005, involved 605 veterans — most of whom were white men with an average age of 64, who had chest or abdominal surgery. All patients received routine postoperative care. Two experimental groups, however, received additional individual attention from a massage therapist: One group got a 20-minute visit, during which the patient and the therapist talked but no massage was given, and another group received a 20-minute back massage for up to five days following their operations. The massage group, the study found, reported markedly less intense and less unpleasant pain and less anxiety than patients who got standard pain medication or individual attention but no massage. Dr. Daniel Hinshaw, a surgeon in the VA Ann Arbor Healthcare System and one of the study's co-authors, says that when asked a day after surgery, some patients reported that massage delivered about as much pain relief as a dose from a morphine drip. Hinshaw suggests that massage functions by creating a competing sensation to block pain or by generating endorphin-like chemicals in the body, which reduce pain and promote a sense of well-being. He also notes the crucial — and often forgotten — role of touch in medicine: Human touch can help alleviate anxiety and ease pain. "Patients crave contact," says Hinshaw. "They want some kind of comforting presence."
The new findings come at the end of an eventful year for massage-therapy research. In March, researchers at the University of California, San Francisco, School of Medicine's Osher Center for Integrative Medicine published a study finding that Swedish massage, shiatsu foot massage, and acupuncture helped reduce pain and depression in postoperative cancer patients. An October 2007 pilot study by the Mayo Clinic showed that massage significantly reduced pain levels in patients recovering from heart surgery, prompting the internationally renowned treatment center to bring a full-time massage therapist onboard. That same month, the American Massage Therapy Association published a survey in which 30% of all respondents who had received a massage in the last five years did so for medical reasons — including pain relief, injury recovery, soreness and control of migraines — compared with 22% who sought relaxation and 13% who were merely indulging themselves. The survey also found that nearly one in five respondents had discussed massage therapy with their doctors, and of those who did, the majority said their doctors had encouraged them try it.
Of course, massage is hardly a breakthrough treatment — it's been used for centuries in traditional healing. The UCLA Center for East-West Medicine, which has incorporated traditional Chinese medicine (TCM) and western medicine since 1993, uses massage for most of its 14,000 or so patients each year, who come for treatment of conditions ranging from post-surgical pain to migraines. Dr. Ka-Kit Hui, the center's founder and director, says massage is safe and effective across the board, reflecting one of the core concepts of TCM: using physical methods to help stimulate the body to correct its own chemical flow. "Muscle spasm is not normal," says Hui, whether it's in a recovering cancer patient or an insomniac. "When you take care of that, other conditions can be helped."
It was, in fact, a moment of medical nostalgia that prompted the pilot study that became the foundation for the VA trial. Recalling his days as a surgical resident in the 1970s, Hinshaw says older nurses would regularly give massages to frail, elderly patients prone to delirium on postoperative drugs. The treatment — standard at the time — helped those patients. "But now most of the nurses who practice it are retired," he says, and, now, medical training adheres more strictly to quantitative means of evaluating patient progress. So, patients' individual concerns and worries are sometimes swept aside in the process, preventing them from receiving proper pain diagnoses, while certain holistic treatments are less likely to be accepted than conventional western practices. "We'd have to stop practicing medicine" if everything doctors did required back-up by evidence from trials, says Hinshaw, "but we have that evidence for massage. We can see a real effect."
Getting the larger health care system to buy into the idea is another matter. Currently some, but not all, U.S. health insurers cover some form of massage therapy. To gain broader, more mainstream acceptance, Hinshaw says, the treatment will have to prove cost-effective as a pain-reliever. But, in most hospitals, where patients are cycled through intensive care units in a "highly choreographed sequence," there's not a lot of time or imagination to squeeze in massage therapy. Further research, perhaps showing that massage can shorten patients' hospital stays or reduce their analgesics use, may prompt hospitals to include massage more routinely in patient care. In the meantime, patients who want the health industry to think outside the box have to say so: If patients demand massage, Hinshaw says, "hospitals will listen."
