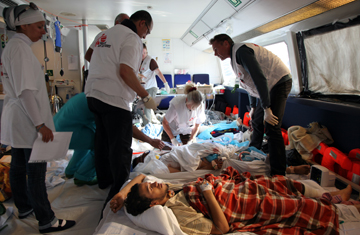
Medics from Doctors Without Borders offer their services on April 16, 2011, in Libya, where NGOs are preparing for a potential mental-health crisis
In the wake of Colonel Muammar Gaddafi's death, Libyans are reveling over the chance to create a new nation, rid of corruption and oppression. But after the streets are emptied and the echo of celebratory gunfire fades, Libyans will also have to rebuild. They will need to restore war-torn towns and repair social and political infrastructures — and they will need to find a way to mend the national psyche.
The war has been wearing on the Libyans. Children are acting out in school; they're agitated and aggressive, sometimes despondent and withdrawn. Teenagers are losing their hair, developing manic symptoms over their worries of what the future brings. And mothers cannot recall how to cook simple recipes, consumed as they are with thoughts of relatives who perished on the front lines.
While the 6.4 million Libyans try to recover from nine months of bloodshed, they also have to cope with the psychological aftermath of nearly 42 years of repression, leaving some experts bracing for an overwhelming need of mental-health services — which isn't helped by a severe shortage of trained staff. In the hopes of staying ahead of a potential mental-health crisis, nongovernmental organizations like Doctors Without Borders and International Medical Corps are already taking steps to help the newly freed population recognize the problems it will have to face.
Last May, three months into the country's civil war, Doctors Without Borders set up support in three hospitals in Misratah to assist caretakers with the influx of patients, whose cases included stress-induced miscarriages and psychosomatic pain. Nathalie Severy, a mental-health expert with Doctors Without Borders, says the organization began training local Libyan psychologists about the emotional consequences of the conflict while also supervising their daily practice. "There was no mental-health system at all before the conflict," she says. "They didn't have any clinical experience."
Dr. Sarah Elhady, 26, a Benghazi native and junior psychiatrist who graduated from medical school last October, concedes that she lacked the clinical practice necessary to deal with a postconflict society. Elhady, a program officer for International Medical Corps, says psychological support was essentially nonexistent before the war. Libyans stigmatized mental-health services, which were only available in the country's two psychiatric hospitals in Tripoli and Benghazi. Those hospitals treated only the most extreme cases, often as last-resort efforts by patients who had been failed by general medical doctors.
But as conflict roiled, psychologists began to take an active role, asking for more training and volunteering at community clinics. International Medical Corps offers a two-day psychological first-aid program to educate first responders and health care providers on how to deal with stress reactions — anxiety, hopelessness, nightmares, physical pain — as well as to train teachers and parents on how to help children cope with their feelings about the war. The program has trained over 300 Libyans so far, says Dr. Inka Weissbecker, an adviser with International Medical Corps. But keeping up with the demand has been difficult.
