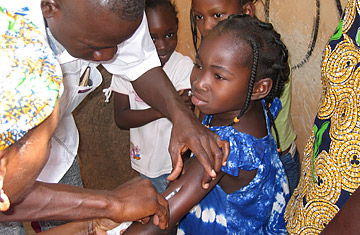
A man vaccinates a girl against meningitis in a medical center in Ouagadougou, Burkina Fase, 23 March 2007
Correction Appended: December 7, 2010
All vaccines are designed to save lives, a lesson the people of Africa will learn anew on Monday when a new meningitis A vaccine is released in Burkina Faso, eventually protecting hundreds of millions of people from a disease that can deafen, disable and often kill its victims. But this vaccine does something else: it demonstrates a whole new way to develop pharmaceutical products quickly and cheaply in the developing world — a place drugs and vaccines are often needed the most, but are hardest to get.
Meningitis A is a selective disease, posing the greatest threat both in particular parts of the world and in particular seasons. It hits the hardest in what is known as the "meningitis belt," a sweep of 25 countries with a combined population of 450 million people, stretching from Senegal in West Africa to Ethiopia in the east. For reasons scientists don't fully understand, the bacterium is most common during the region's dry season, which begins in January and ends in March. An epidemic last year killed 4,053 people in 14 countries, and a total of 78,416 were infected. A 1996 outbreak infected a quarter of a million.
The vaccination program that begins next week will take aim at this scourge first by inoculating 12.5 million people aged one to 29 in Burkina Faso — a country that that lies near the center of the meningitis belt and has one of the highest infection rates on the continent. By the end of the year, the World Health Organization (WHO) plans to have reached 20 million people by expanding into Mali and Niger. By 2015, it hopes to have the entire meningitis belt covered. Immunizing half a billion people in under five years would be a public health coup by any measure, but the way the new vaccine — called MenAfriVac — came to be makes the achievement all the more significant.
Western drug companies traditionally pour hundreds of millions or even billions of dollars into developing a new drug or vaccine, not least because of the decades of research it can take to prove the product both safe and effective. Those costs are reflected in the price: existing meningitis vaccines, for instance, currently retail for around $120 per dose. That prohibitive cost puts many medicines out of reach in the developing world. And when the developing world is the only place a particular disease — such as dengue fever — exists, needed drugs may never be developed at all, since the companies know they'll never recoup their sunk costs.
"Africa just isn't a good market for drugs," says Marc LaForce, director of the Meningitis Vaccine Project (MVP), which developed the MenAfriVac.
That often leads to unseemly — even ugly — clashes between the companies that control the access to lifesaving medications and the people who need them most. Tachi Yamada, global health director of the Gates Foundation, which bankrolled MVP with $90 million in grants, left his former position at GlaxoSmithKline when, as he says, "we sued Nelson Mandela," a reference to the legal action taken by Western drug companies at the turn of the millennium against South Africa for distributing cheaper generic HIV/AIDS drugs.
MVP has reinvented the vaccine-development wheel in a number of ways. For one thing the organization spent just $50 million to develop MenAfriVac; for another, it moved the product from lab bench to consumer in just six years. Last, and most significant, it has been able to price a single shot of the vaccine at less than 40 cents. The developers achieved all that in part by building the vaccine out of the pharmaceutical equivalent of off-the-shelf parts.
The work started with an existing meningitis vaccine that is effective but limited — providing protection that lasts only about a year. Scientists then found a drug company that was willing to part with a patented method of creating a longer lasting conjugate vaccine, created by combining the vaccine with a tetanus protein. Introduced into the body, the tetanus provokes a more vigorous immune response, fortifying the effect of the overall vaccine. In 2003, these two technologies were transferred for synthesis and mass manufacture to the Serum Institute in India, whose lower cost base ensured the vaccine would be cheap. On Monday, the commercial product that resulted from all this innovation will be in use. "In drug development terms, that's warp speed," says LaForce.
The hope is that this new, cut-price model of drug development can be adapted to other diseases of the developing world too, such as pneumonia and rotavirus, both of which are already in the Gates Foundation's sights as the next targets of cheap and streamlined vaccines. The cruel irony of the battle for global health is that the diseases that claim the greatest number of lives in the developing world have long since been tamed or beaten in developed countries — a kind of geographic lottery that public health officials have always seen as insupportable.
"The only thing worse than not having a vaccine is having a vaccine that you cannot afford," says Chris Elias, president and CEO of PATH (the Program for Appropriate Technology in Health), which pioneers public-private efforts to develop drugs and is a partner of MVP. "[MenAriVac] is a great vaccine, it's very inexpensive, there's a huge demand for it and it's the first vaccine ever developed for the African market. It's amazing."
The original version of this story misidentified the cause of Meningitis A as a virus. The disease is caused by a bacterium.
