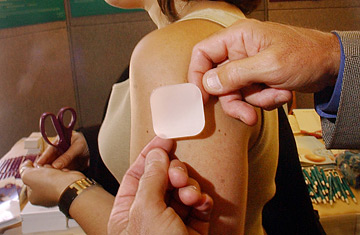
LA JOLLA, CA - SEPTEMBER 12: Becca Dillur models an Ortho Evra contraceptive patch September 12, 2003 at the Association of Reproductive Health Professional convention in La Jolla, California. The Ortho Evra is a weekly contraceptive patch that slowly releases Estrogen into the body through the skin.
When is it a good time to take estrogen? Every new study on hormone replacement therapy and menopause seems to confuse the question further. Taking estrogen and progestin has been linked to increased risks of heart disease, stroke and even breast cancer in postmenopausal women. But what about taking estrogen alone, for women who have had their uterus or ovaries removed? Studies have suggested that there's a critical, age-dependent window before menopause during which the hormone — either the body's natural estrogen or that which is introduced during therapy — is protective. Now, two new, related studies in the Aug. 29 online edition of Neurology lend more support to that theory: these studies show that in women under 50, estrogen acts as a defense against later cognitive impairment, dementia and Parkinson's disease.
The larger of the two studies — a broad review of data from about 3,000 interviews with women in Olmsted County, Minn. — is among the first to show that ovarian preservation and estrogen therapy protect brain function. Of the study participants, who were all matched for age, 813 women had one ovary removed and 676 women had both ovaries removed, while the 1,472 women in the control group had both ovaries intact. Half of the women had oophorectomies because of a benign condition, such as infection or cysts, and the other half had their ovaries removed prophylactically to prevent ovarian cancer. Lead investigator Dr. Walter Rocca, a neurologist and epidemiologist at the Mayo Clinic in Minnesota, and his team found that compared with women who had kept both ovaries, the risk of cognitive impairment or dementia was doubled in women who had both ovaries removed before age 48 or one ovary removed before age 41.
"The younger the age of the woman at the time of oophorectomy, the higher her risk of cognitive impairment or dementia because there is a longer period in which she is deprived of estrogen and neuroprotection," says Rocca. "Our study suggests that if there is good reason to remove the ovaries before age 50, there is good reason to consider [estrogen] treatment until 50, the age when a woman naturally reaches menopause."
While its general findings are valid, Rocca's study had limitations. For instance, the participants' dementia was measured not in person, but through a cognitive test over the phone or through a proxy. Also, the women had had their surgeries between 1950 and 1987 — oophorectomy procedures and estrogen therapy may have been different then than now.
Rocca and his group conducted a second, more comprehensive study with the same women. With better funding this time, researchers were able to examine patients in person in order to study the impact of ovary removal on movement disorders, such as Parkinson's disease. Again, the researchers found a powerful effect: when ovaries were removed at a relatively young age, the risk of Parkinson's disease increased. For women who had both ovaries removed before age 48, there was an exact doubling of risk compared with women with intact ovaries.
The link between protective mental health benefits and estrogen therapy appears to conflict with the findings of the Women's Health Initiative (WHI), which found that women who took estrogen alone or estrogen plus progestin from age 65 increased their risk of mild impairment or dementia — along with other cardiovascular problems. But the authors of the Neurology studies stress that the age-dependent window is key when considering therapy and mental health. "Below 50, estrogen is protective. After 65 it is harmful. But nobody really knows between 50 and 65," says Rocca. "In the middle it's still unclear."
Dr. Lynn Shuster, director of the Women's Health Clinic at the Mayo Clinic, agrees that timing is crucial. The women in the WHI study were years out from menopause and probably already had significant hardening and narrowing of the arteries, says Shuster. It comes as no surprise, then, that taking an estrogen pill, which increases blood clots, would increase heart and brain events. "The problem is that the results of the WHI were extrapolated to say that older women shouldn't take estrogen. But the bigger issue probably depends on when a woman starts it, if it is going to be protective or harmful."
In April, another WHI study published in the New England Journal of Medicine found that estrogen-alone therapy benefited women between ages 50 and 59 who had had hysterectomies; these women had up to 40% less calcified plaque build-up in their arteries compared with women on a placebo. In the coming years, other trials, such as the Early Versus Late Intervention Trial With Estradiol (ELITE) and the Kronos Early Estrogen Prevention Study (KEEPS), will provide more data on estrogen's effect on women's health, particularly cardiovascular health, says Rocca.
For now, however, his new studies may well change standards of care. Women who are considering a hysterectomy or ovary removal now also need to be aware of the increased risk of dementia, says Shuster, who encourages patients who have had a hysterectomy and oophorectomy at a young age to take estrogen until the natural age of menopause, if not beyond. "The big news is that we shouldn't be withdrawing estrogen from women who need it," says Shuster. "Medically, legally, there is an exaggerated fear of prescribing estrogen, and women have a fear of taking estrogen because of all the bad news. Women are now coming off of it at too a young an age and having increased osteoporosis and increased heart problems and now potentially increased dementia or Parkinson's."
